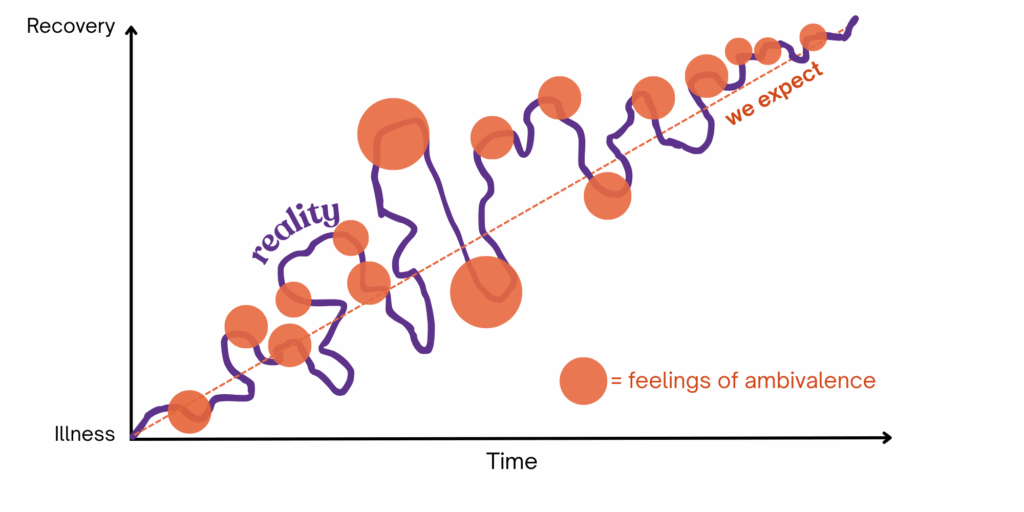
Name your feelings and emotions. What’s going on for you right now? How do you feel when you are motivated to recover, and how do you feel when you want to stay with the eating disorder? It can help to share this with a trusted loved one or treatment professional. Even just sharing with one person can help you feel less alone.
Be kind and gentle with yourself. Recovery is not linear. It takes time, and it can often be challenging. Remember to be patient with the process and not be hard on yourself.
Find things which bring you joy and incorporate them into your day. Whether that be a swim at the beach, lighting a candle, a warm cup of tea or talking to your best friend on the phone. Creating distance, even for short moments, between you and the eating disorder is vital to overcome ambivalence.
Identify what you want outside of the eating disorder. This may include:
- writing a list
- creating a vision board
- journalling about of all the things you want to do in your life which are out of reach while you have the eating disorder.
Looking beyond the eating disorder can give you a sense of purpose for recovery. It gives you something else to set goals around and focus on.
Connect your loved ones with EDV so they can get some tips on how to best support you during these times.
Find a mental health professional with expertise in eating disorders, and/or a peer worker. This should be someone who you feel safe to open up to and talk to about your ambivalence.
“At the time I was most ambivalent, I was throwing myself into work and study. This led me to experiences that eventually strengthened my resolve to recover, but being so busy made it hard to do the self-reflection and self-care I needed.
“However, I started learning about the concept of self-compassion at this time, and started learning that you could change the way you spoke to yourself, your ‘inner voice’ and intentionally use kind, compassionate and soothing language in times of distress. This started building up a bit of confidence and trust in myself.
“I was also learning about the true needs of the body energy-wise – and experiencing how trying to hold onto disordered habits meant being ‘at war’ with my mind and body, and feeling how that was in direct opposition to the one I was attempting to cultivate internally.”
—Anonymous
“A big [thing that helped move me out of ambivalence] was information. Understanding the science behind eating disorders and recovery and that there were paths to recovery; that lots of people before me had reached recovery, reading their stories.
“For me it was also understanding and accepting that my body had a natural weight-set point and I needed to rest and refeed to find freedom.
“But I think ultimately it was my values peeking through (and becoming clearer through different experiences) that gave me the strength to continue with recovery despite this ambivalence and questioning.
“I didn’t want to simply ‘succeed’ in these narrow and damaging ways. I wanted to be a present friend, have healthy relationships, care about wider world issues again, and experience life to the fullest. I wanted to stop harming myself, stop struggling and start living — to give myself the best chance at living a good life.”
—Anonymous